
IVF in Brief
IVF is popular because it “short circuits” many of the natural processes needed to make a baby. Many of these steps are still poorly understood and their relevance in slowness to conceive is often uncertain.
The “by-pass” strategy of IVF can therefore be an effective solution for a wide variety of fertility problems. This does not mean that IVF is always needed. Sometimes there are other, simpler alternatives.
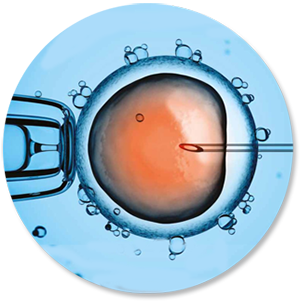
IVF involves
- Stimulating the ovaries with a medicine called FSH for about 10 days. A tiny self-administered needle is used. Work can continue.
- About every 3 days an early morning visit is needed at one of the Genea sites (scattered widely over Sydney and NSW). A blood test, and sometimes an ultrasound, is performed.
- It is rare to see anyone drop out of treatment because of FSH side-effects.
- After about 10 days, a day needs to be taken off work for an egg collection. Collection is done with a guided needle on a vaginal ultrasound probe. It takes about 15 minutes.
- You can elect to have local or general anaesthesia.
- The eggs are fertilised in the lab with your partner’s sperm.
- After 3-5 days a single embryo is placed in the womb with a thin catheter. This is like having a Pap smear.
- A pregnancy test is done 11 days later.
- Any spare embryos are frozen. These can be used later if needed.
- High quality, comprehensive IVF units like Genea have excellent freezing technology as well as Pre Implantation Genetic Screening (PGS), the ability to check embryos for common abnormalities before transfer.
The chance of a baby from a first embryo transfer ranges from 5 to 50% with women under 40 doing much better than women over 40.
With PGS, pregnancy rates of 60% per transfer are common. The chance of a major complication from IVF is low and less than the risk of pregnancy complications.
IVF is well-tolerated by most women although it can be emotionally taxing at times and it does entail significant effort, but, if it is statistically your best chance of success, it makes sense to “just do it”.
IVF at a top unit is more expensive, but certainly cost-effective because of higher success rates and a much greater level of personal attention and support.
Lots of cycles at cheap units with relatively poor success rates, or other treatment strategies that are just speculative, often prove, in hindsight, to be the harder, more costly and less productive options.
For an appointment to discuss IVF, please call Sarah (02) 9221 2904